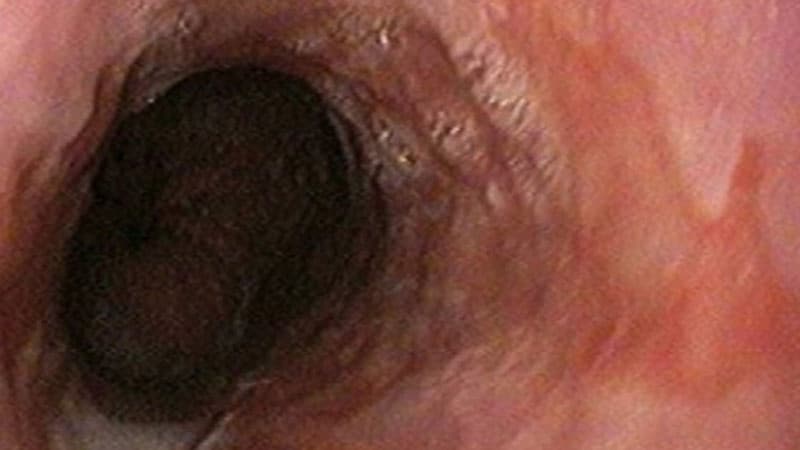
A new clinical practice update from the American Gastroenterological Association offers practical advice around surveillance and use of new screening technologies for Barrett’s esophagus.
The AGA clinical practice update, published in Clinical Gastroenterology and Hepatology comes from the AGA’s Center for GI Innovation and Technology. It offers 15 best practice advice statements based on expert review of existing literature combined with discussion and expert opinion. The aim is “to provide an update on advances and innovation” but not to replace current guidelines.
“Guidelines operate on rigorous methodology which requires the use of [Grading of Recommendations, Assessment, Development and Evaluation] methodology and a higher level of evidence. In gastroenterology especially, innovation is moving quickly and there’s no way for patients to reap their benefits if clinical practice was dictated by guidelines alone. That said, we do need documents that support and drive innovation in clinical practice,” corresponding author Srinadh Komanduri, MD, professor of medicine and surgery in the division of gastroenterology and hepatology at Northwestern University, Chicago, told this news publication.
Asked to comment, Vivek Kaul, MD, the Segal-Watson Professor of Medicine in the Center for Advanced Therapeutic Endoscopy in the division of gastroenterology and hepatology at the University of Rochester (N.Y.) Medical Center, said that the document is “an important attempt to not only present the available scientific literature in a very concise and understandable manner, but it goes above and beyond that in terms of diving into some novel paradigms and technologies and procedures that are either emerging or will be emerging in the near future.”
Improving Detection by Dropping GERD Requirement
The first of the 15 statements may also be the most paradigm shifting: The panel suggests screening via standard upper endoscopy of people with at least three risk factors for Barrett’s esophagus and esophageal adenocarcinoma, including those who are male, are non-Hispanic White, are aged above 50 years, and have a history of smoking, chronic gastroesophageal reflux disease (GERD), obesity, or a family history of Barrett’s esophagus or esophageal adenocarcinoma.
This represents a departure from all current guidelines, which stipulate GERD as a necessary prerequisite for screening. But the reason is simple, according to the authors: A majority of patients diagnosed with esophageal cancer never experience classic GERD symptoms.
“There is growing evidence in high-level publications over the last couple of years that reflux is not the ideal predictor, based on odds, for development of Barrett’s esophagus. So the consensus among the experts was that we need to remove GERD as an absolute prerequisite or we’re never going to make progress. In order to make an impact on the rise of esophageal adenocarcinoma we have to increase the denominator of patients we are seeing,” Komanduri explained.
While it might be difficult to screen every White male over 50 years of age, the data do suggest screening those who also have obesity and/or are current smokers. “That’s a perfect subset you might want to start with. There are permutations that have greater value that don’t occupy unnecessary resource utilization. Most critical are the family history of esophageal cancer or Barrett’s esophagus,” he noted.
Kaul said that a one-time Barrett’s esophagus screening of all White males over 50 years old “is not unreasonable, especially given the rising rates of esophageal cancer.”
However, he also noted, “The feasibility, preferred screening modality, incremental costs, and yield of this new strategy will need to be studied further. Access to GI endoscopy in the postpandemic world is already a concern and will need to be factored into execution of this [advice statement] and will likely impact adoption in some way.”
For his part, Komanduri said that more investigation will be needed to validate which patients most benefit from screening and that the AGA is planning educational programs for clinicians about interpreting this new paradigm.
New Technology Could Make Screening Easier and Cheaper
The availability of nonendoscopic cell collection devices, including the swallowable Cytosponge (Medtronic), EsoCheck (Lucid), and EsoCap (Capnostics) could help make screening for Barrett’s esophagus easier and more cost effective. They are designed for in-office use and don’t require sedation. Each one is currently in various stages of development and clinical trials. As of now they’re approved in the United States only for cell collection but not for Barrett’s esophagus screening, but their use is endorsed by some guidelines. The Cytosponge in particular is widely available and has been used extensively in the United Kingdom.
Kaul commented, “While there is a need for nonendoscopic screening devices, the ideal patient population and practice setting for administration of these devices has not been clearly defined. Also, who will be delivering these tests: Primary care or gastroenterology providers? These devices … represent a major step forward and a novel paradigm for Barrett’s esophagus screening, and the only platform that non-GI providers could use.”
Virtual Chromoendoscopy: A Must Have in 2022
A third best practice advice statement shouldn’t be controversial because it’s in other guidelines already, but data show clinicians aren’t always doing it: Performing screening and surveillance endoscopic examinations using virtual chromoendoscopy in addition to high-definition white light endoscopy, with adequate time spent inspecting the Barrett’s segment. The majority of data supporting this is for narrow-band imaging only.
“The blue light lets you pick up early mucosal and vascular changes which might represent dysplastic lesions. It’s not a question of should. It’s a medicolegal slam dunk; you must do it. It’s been a guideline recommendation in the last few years, and it’s just a switch on the scope. It doesn’t require separate equipment, yet people are often still skipping it,” Komanduri said.
Indeed, Kaul concurred, “The importance of a high quality, meticulous endoscopic examination for screening and surveillance in Barrett’s esophagus cannot be overemphasized.”
“Finally Pushing the Needle in the Right Direction”
The overall goals, Komanduri said, are “increasing the denominator, using less invasive screening, but finding more patients. If we find more patients we’ll need to stratify their risk. We hope that all these things eventually tie together in a nice story, all with the aim of preventing an invasive cancer that can’t be treated.”
He believes the new update “is a pivotal document in this field that’s going to be a paradigm changer. A lot of aspects need further validation. It’s by no means the end. But I think we’re finally pushing the needle in the right direction as things move forward with innovation.”
Kaul agrees. “It’s highlighting the principles that may become established paradigms in the future.”
Komanduri and the other authors of the update reported relationships, including consulting and research support, with companies like Boston Scientific, Medtronic, Virgo Video Solutions, and Castle Biosciences. Kaul serves as a consultant and advisory board member for CDx Diagnostics, an advisory board member for Castle Biosciences, and an investigator for Lucid Diagnostics.
This article originally appeared on MDedge.com, part of the Medscape Professional Network.
Source: Read Full Article