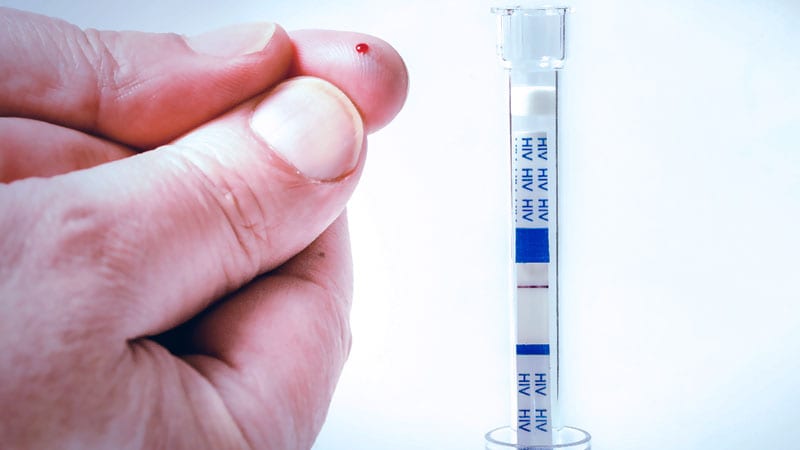
MADRID — Rapid tests for the detection of the human immunodeficiency virus (HIV) shorten the window period to 2 or 3 weeks, and self-tests are as reliable and accurate as those carried out by healthcare workers. Both are essential in strategies to increase the rate of diagnoses. Uncertainties when managing people with HIV relate to questions such as when to start therapy, drug interactions, treatment adherence, and the aging of this population.
María Jesús Pérez Elías, MD, PhD, head of the Infectious Diseases Department of the Ramón y Cajal University Hospital in Madrid, provided an update on early diagnosis of HIV at the 43rd Congress of the Spanish Society of Internal Medicine. She introduced the topic with epidemiological data on HIV in Spain.
According to the General Office of Public Health, Quality, and Innovation – National Epidemiology Center of the ISCIII of Madrid, prevalence improved in 2020 compared with 2017, “although we do not know if it is the result of underdiagnosis and underreporting, and whether they are reliable figures,” said Pérez Elías. The epidemic seems to be focused on the following territories and groups: Catalonia, Madrid, Andalusia and Valencia, non-Spanish patients, and men who have sex with men. Half of new diagnoses are among patients outside these groups, however.
In the data published in 2017-2019, 151,387 people in Spain were living with HIV. Of this group, 87% had a diagnosis, 97% were in treatment, and 90% had viral suppression, although “a very simple count tells us that 39,897 people are at risk of progression and transmit the disease,” said Pérez Elías. Half of new diagnoses are made late, and there has been no progress in this regard in recent years. This circumstance has negative consequences for the patient and a negative impact on the control of the epidemic.
The two clear objectives are to prevent new infections and, for those that have already occurred or are occurring, to diagnose them as soon as possible after the primary infection. “Eighty percent of infections are caused by people who are unaware of their situation,” recalled Pérez Elías.
The strategies and actions to achieve the objective are described in the National Plan for HIV/sexually transmitted (STIs)/hepatitis C virus (HCV)/tuberculosis infections. The document advocates the early diagnosis of HIV infection and other sexually transmitted infections to ensure that all people with HIV know their HIV status; to detect a greater number of people with HIV; and to incorporate the latter into early care and treatment, thus breaking the chains of transmission.
To achieve this objective, it will be necessary to increase knowledge about the care and prevention infrastructures in Spain. Clinicians also must promote HIV testing and link the diagnosis of HIV to the initiation of antiretroviral therapy (ART). In addition, studies of infected patients’ contacts must be reinforced.
Risk-Based Guidelines
There are several specific guidelines based on exposure risks. Among other populations, they focus on the sexual partners of people with HIV; men who have sex with men and their partners; people who have suffered a sexual assault; others who want to stop using condoms with their stable partners; people with occupational, sexual, or accidental exposure risk to HIV; and people from countries with high HIV prevalence (greater than 1%) and their sexual partners.
The past decade, recalled Pérez Elías, has witnessed four DRIVE studies (Rapid Diagnosis of HIV Infection in Spain). The last one, ATENEA 2022, focused on eight health centers with HIV-HCV risk identification. “These programs really work,” she said. The prospective observational DRIVE 01, when compared with routine, increased the rate of new HIV diagnoses ninefold in the emergency room and 24-fold in primary care. Screening coverage increased fivefold in the emergency room and sevenfold in primary care.
DRIVE 03, randomized, when compared with the usual routine, increased HIV and HCV screening rates 10-fold, and rates of new HIV diagnoses were multiplied two- and fourfold with respect to HCV.
Rapid Tests
Rapid HIV diagnostic tests are classified as third generation, which detect antibodies against HIV-1 and HIV-2 types from three weeks after infection, or fourth generation, which detect, in addition to the previous antibodies, the HIV-1 p24 antigen. “These latest serological techniques shorten the window period to 2 or 3 weeks after infection, because they include the detection of p24 antigen,” said Pérez Elías.
She highlighted data from a review that are favorable to these tests. Between 40% and 90% of people prefer rapid tests over conventional ones, and if they could choose, 87%-97% would opt for the rapid tests. It is estimated that for 10%-52% of people who take an HIV test, it is the first time they have been screened. The percentage of people who receive their result after being tested varies between 27% and 100%, depending on the risk group. Among the people who test positive, 70%-100% undergo the HIV confirmation test, with high rates of link-up to care (22%-100%) and satisfaction with the experience (70%-99%).
On the other hand, the World Health Organization recommends carrying out tests outside the health system. It urges the use of HIV tests aimed at populations at greatest risk. Pérez Elías discussed the screening and link-up of HIV infection in non-healthcare settings. The HIV test can be carried out in nongovernmental organizations, places close to the population, or at the person’s own home. “Testing in these settings offers an effective way in addition to linking very vulnerable people like drug users and immigrants.”
Addressing Uncertainties
Antonio Antela López, MD, PhD, of the University Clinical Hospital of Santiago de Compostela, Spain, described uncertainties that are encountered frequently when managing patients with HIV. For example, it is not known what the patient is like when they first attend a consultation and start ART. The willingness and motivation of the patient are critical factors in the decision to start treatment. Also, “it is essential to make an individualized assessment both of the time of initiation and the drugs that will be part of the initial [therapeutic regimen],” said Antela López.
The uncertainties at the time of starting the initial ART are diverse, since the therapy must be easy to take, be well tolerated, and not require prior testing (such as HLA B 5701, resistance test, hepatitis B virus serology, viral load, CD4+ lymphocyte level). Furthermore, it must entail minimal risk of drug interactions and a high barrier against resistance. “An effective, simple, well-tolerated, robust ART with few interactions, such as B/F/TAF [bictegravir/emtricitabine/tenofovir alafenamide], can be used by most people with HIV and makes their lives easier,” said Antela López.
Multiple Interactions
Other uncertainties arise when accounting for interactions with drugs commonly used in these patients, such as lipid-lowering agents, anxiolytics, antidepressants, antacids, or antihypertensives. In addition, there are also interactions with the main recreational drugs, including amphetamines, ecstasy, ketamine, lysergic acid diethylamide (LSD), and mephedrone. Similarly, the habitual excessive consumption of alcohol should not be underestimated as a cause of inadequate compliance with treatment, nor should the consumption of herbal or parapharmacy products be forgotten. Therefore, “it is a priority to choose ART with fewer drug interactions,” said Antela López.
He stressed the uncertainties that arise from inadequate therapeutic compliance, since the probability of experiencing a period of low compliance increases over time (almost 50% at 3 years). It has been reported that as many as 60% of patients do not adhere to their ART, thus increasing the risk of virologic failure and the emergence of resistance. Viral rebounds are also frequent (23%) and double the risk of virologic failure.
Given the interactions, it should be remembered that in Spain, 32% of people with HIV suffer from psychiatric disorders, the most common being anxiety and depression. Depression occurs in 39% of people with HIV, which in turn is correlated with lower adherence to treatment.
More uncertainties arise from risky sexual practices such as “chemsex” (the consumption of drugs to facilitate/enhance sexual activity), which constitutes a significant barrier to optimal compliance with ART. In some places, almost 15% of men who have sex with men practice chemsex.
Elderly With HIV
The aging of the population with HIV is associated with an increase in comorbidities, which gives rise to polypharmacy. “We have to pay more and more attention to the screening and management of comorbidities, so it is essential that ART be as stable as possible,” added Antela López.
Patients with HIV infection are considered elderly from 50 years of age, and it is estimated that there are more than 17.5 million people with HIV in that age group — but they are not all the same. Frailty is a clear predictor of health events and mortality from any cause. Therefore, “an elderly person with HIV is complex, but not homogeneous, so the objective should be to detect those who are vulnerable,” said Antela López.
A study of frailty and physical function in a Spanish cohort of patients older than 50 years with HIV infection (FUNCFRAIL Study) was published in PLOS One. The study of the multicenter cohort, from 11 Spanish hospitals with a 5-year follow-up, includes baseline data on HIV infection, comorbidities, polypharmacy, comprehensive geriatric assessment (physical function, gait speed), frailty (Fried phenotype), and laboratory tests (blood, urinary, and coprological). The study shows that aging is not homogeneous. Patients over age 65 years are different (they live alone and have typical comorbidities) from long-term HIV survivors (mainly women; more years of life with known HIV, depression, and psychiatric disorders).
Pérez Elías and Antela report no relevant financial relationships.
Follow Javier Cotelo of Medscape Spanish Edition on Twitter @Drjavico .
This article was translated from the Medscape Spanish edition.
For more news, follow Medscape on Facebook, Twitter, Instagram, YouTube, and LinkedIn
Source: Read Full Article