The list of diseases caused by SARS-CoV-2 infection is growing and now includes the retina. This is what is suggested by a prospective study by the Geneva University Hospitals (HUG) and the University of Geneva (UNIGE), in collaboration with the Adolphe de Rothschild Memorial Clinical Research Center for Ophthalmology. This research reveals that 11% of people hospitalized for respiratory distress due to COVID-19 disease have retinal damage. This study can be found in the Journal of Clinical Medicine.
Since the first pandemic wave of SARS-CoV-2, scientists and physicians have observed neurological and vascular damage in infected individuals. Since the retina is part of the nervous system and offers a direct and non-invasive observation pathway to the vessels, a research team from the HUG, the UNIGE and the Adolphe de Rothschild Memorial Clinical Research Centre in Ophthalmology performed fundus examinations on patients admitted to the HUG Internal Medicine Department for pneumonia due to COVID-19 and placed on oxygen therapy.
“A photograph of the back of the eye gives access to the vascular system of the retina, a godsend for studying COVID-19 vessel disease in an easy way,” says Eleonora Riotto, then a student at the UNIGE Faculty of Medicine and the first author of this study that takes into account 172 people infected with SARS-CoV-2.
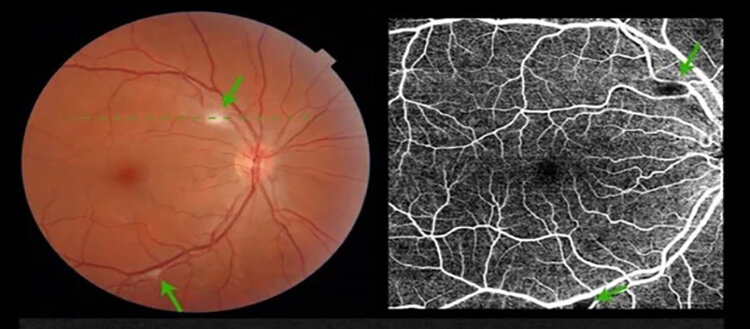
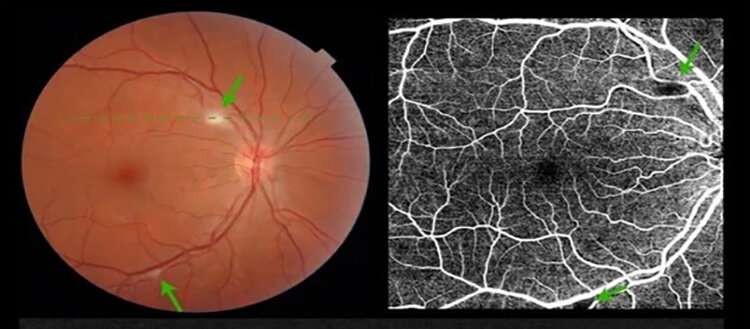
White spots on the retina
The research team performed these examinations using a camera that photographed the retina without pupil dilation. These examinations revealed white spots on the retinas in 11 percent of cases. “These spots are known as cotton wool spots. They are signs of retinal suffering secondary to small artery occlusion. They can be caused by embolism or inflammation of the retinal vessels, with vasculitis creating an obstruction to blood circulation and potentially a lack of oxygen and nutrients. They are mostly seen in people with diabetes or hypertension,” says Dr. Gordana Sunaric Mégevand, medical director of the Adolphe de Rothschild Memorial Clinical Research Center for Ophthalmology and the study’s final author.
An alteration correlated with COVID-19
These data were then cross-referenced with the health status of the individuals and their symptoms. A history of diabetes, overweight, and elevated C-reactive protein—whose expression reflects inflammation following infection or tissue damage—were more frequently observed in patients with cotton wool spots. However, although there was a correlation with diabetes, the study showed that nearly 64% of the participants with retinal abnormalities did not previously have diabetes.
The same was true for hypertension, since nearly 90% of the patients with retinal damage had no history of hypertension to explain this phenomenon. “Our results therefore argue for a retinal alteration mainly due to viral infection, although cotton wool sports are known to be the first ophthalmological finding of diabetic or hypertensive retinopathy,” said Dr. Christophe Marti, assistant physician at the HUG’s Department of General Internal Medicine, private doctor at the Department of Medicine of the Faculty of Medicine of the UNIGE and co-author of the study.
The research team then reviewed each patient three months after hospitalization. They found that all the spots had disappeared and that no one had any vision problems. “The study participants will be followed up to confirm these reassuring findings,” says Dr. Gordana Sunaric Mégevand.
Three possible causes
The study does not investigate the causes of these transient retinal injuries. Nevertheless, the research team believes that three different mechanisms could explain them. First, direct tissue damage by virus infiltration into the endothelial cells of vessels could cause inflammation and vascular obstruction. A second explanation is the potential occlusion of retinal arterioles caused by a state of hypercoagulability in relation to the deposition of fibrin clots observed in many studies with COVID-19.
The last hypothesis suggests that the cotton wool spots occur as a result of under-oxygenation related to the acute respiratory distress of the study subjects or the elevated blood pressure typically seen in the early phase of COVID-19 disease.
Source: Read Full Article